2024/07/27 printed from http://dermboard.org All Rights Reserved

What is melanoma?
Melanoma is a cancer made of cells that give color to the skin which are called melanocytes. Melanoma is one of the deadliest skin cancers. It may occur on any part of the skin, in the eye, in the mouth, on genitalia and rarely on other body parts. It can occur on normal looking skin, or it can occur near, or within an existing mole. It is usually caused by exposure to ultraviolet radiation (sun and tanning beds), and it can run in families. It can occur in any race, but it is most common in Caucasians. The number of new melanoma patients has been increasing for the last 30 years. Melanoma can spread to other parts of body and internal organs, which can be deadly. One American dies of melanoma every hour. However, 98 out 100 people with melanoma will survive at least 5 years, if their melanoma is treated before it spreads. Therefore, it is very important to catch melanoma as early as possible.
How can I recognize or detect melanoma on my skin?
In most cases melanoma looks like a brown/black spot, or bump on the skin with irregular color and/or shape. Usually it doesn’t feel like anything, but sometimes it can bleed, itch, or be painful. It can also develop from a normal mole which started changing colors, shapes, size, or that has become painful, itchy or started bleeding. Very useful is ABCDEF melanoma rule (see your health care provider if any is present):
- A stands for Asymmetry – One part does not look like the other part.
- B stands for Border – Jagged, scalloped or uneven edge or border.
- C stands for Color – Has different colors (different shades of brown, black, white, blue and/or red).
- D stands for Diameter – It is larger than the eraser at the end of a pencil (but it can be smaller).
- E stands for Evolving (i.e. changing)  – Changing its size, color, or shape over time.
- F stands for Feel – Itching, pain, soreness (but it can totally be without any feel to it).
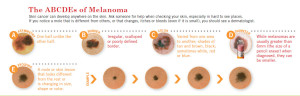
Click on the image to enlarge. Reprinted with permission from the American Academy of Dermatology. All rights reserved.
When should I see my health care provider?
If you notice any mole, spot or bump that has any feature described in the above ABCDEF melanoma rule, you should see your health care provider as soon as possible.

Â
What will my health care provider do?
Your health care provider will listen to your story, and examine the suspected spot. If needed, additional testing will be done such as cutting the entire spot out, or almost the entire spot under local anesthesia for a microscopic examination. Sometimes your health care provider will refer you to a dermatologist for further examination that usually includes examination with a dermatoscope and possibly a biopsy. Dermatoscope is a handheld instrument that looks similar to a battery lamp, but with special system of polarized lenses and LED light that enables your health care provider to take deeper look into the skin. It is usually used by dermatologists. Another name for dermatoscope is epiluminescence microscope. This examination with a dermatoscope may help to avoid the biopsy in some cases, so seeing a dermatologist is a worthwhile of trouble.

OK, I have just been diagnosed with melanoma, but what now?
If you have just been diagnosed with melanoma the most important finding in the biopsy report is the depth of the melanoma (i.e. how deep it goes into the skin). This depth is called “Breslow thickness” and it is listed in millimeters. The deeper the melanoma is, the worse prognosis is. Further management depends on the Breslow thickness (i.e. depth of melanoma), and can vary from a simple excision under local anesthesia, to a more complex procedure such as sampling of surrounding lymph nodes (medical name is “sentinel lymph node biopsy”), imaging (X-rays, CT scan, PET-CT scan and MRI) and/or blood tests, to see if it has spread to some distant body parts, and possible chemotherapy. A great resource to learn about management of your melanoma is the National Comprehensive Cancer Network (NCCN) web site, that doctors also use to guide them in melanoma management: http://www.nccn.org/patients/guidelines/melanoma   Â
Also, if by now you have not found a board certified dermatologist, this is the time to have one taking care of you ASAP.
I had my treatments, what now?
 You should have regular full-body exams by your board certified dermatologist (e.g. every 3 months for 1 year, then a little bit less often depending on the findings). Also you should check your skin – head to toes, and you should check your lymph nodes every month, and report any changes to your dermatologist. You should also inform your blood relatives about your melanoma diagnosis, so that a board certified dermatologist can also check them.
How can I prevent melanoma?
The best would be to stay away from sun, or at least seek shade between 10 a.m. and 2 p.m., wear lightweight, loose-fitting long-sleeved shirt, pants, a  wide-brimmed hat and sunglasses. In good old times ladies wore gloves and carried parasols as well.  Also avoid use of any indoor tanning devices. Second step would be to generously apply a broad-spectrum sunscreen with a SPF (Sun Protection Factor) of at least 30. Our family favorite is Banana Boat Kids SPF 50  (with titanium dioxide and zinc oxide), which is, by the way, one of the cheapest sunscreens.
Also, avoid any tanning, since tan is a sign of skin’s struggle with a genetic damage caused by the ultraviolet radiation. Not everyone who tans will get skin cancer, but everyone will age much faster. Therefore, if you want to preserve your youthful look, please consider the information above. We also like to point one fact to our patients – The Sun is a humongous nuclear reactor in the sky, and there is only an empty space between you and that nuclear reactor. When you think like that, it is a bit easier to follow the above recommendations. Worth of mentioning is an iconic Slip-Slop-Slap sun protection campaign in Australia during the 1980s.
It stands for:
Slip on a shirt,
Slop on the 30+ sunscreen,
Slap on a hat!
