2024/10/22 printed from http://dermboard.org All Rights Reserved
What is an eczema (atopic dermatitis)?
Eczema is a common name for “atopic dermatitis†where your skin is itchy, red, sometimes bumpy and flaky. There is still debate as to what could be the cause, but it runs in families and in persons who have problems with breathing such as asthma, bronchitis and seasonal allergies. Therefore inheritance plays important role. Contrary to a common belief, eczema is rarely associated with food allergies. It occurs more in children, but it can be present at any age.
What is the cause of eczema (atopic dermatitis)?
The exact cause of eczema is unknown. But, we believe that there is a problem with skin evaporating water too fast in some areas due to a defect in the skin sealant called filaggrin (abbreviation from filament aggregating protein). Wherever there is a problem with this sealant, skin evaporates water too fast, gets dry, it cracks, becomes inflamed and itchy. Itch is actually a low level pain sensation, probably from dry, scaly skin poking itself. When skin becomes itchy, guess what, we start scratching it. Scratching in turn makes things worse by removing or plowing the diseased and surrounding normal skin away, which spreads the rash. In addition no matter how good we wash our hands there are still millions of microbes under our fingernails, and frequently those are the microbes found in the nose (almost everyone pokes their noses). Therefore by scratching we also plow those microbes into the skin, which make the eczema much worse. We also believe that by scratching, your skin gets exposed to various chemicals and substances found in your surroundings, which may cause allergic response, which in turn makes your eczema worse.
How do I know if I have an eczema (atopic dermatitis)?
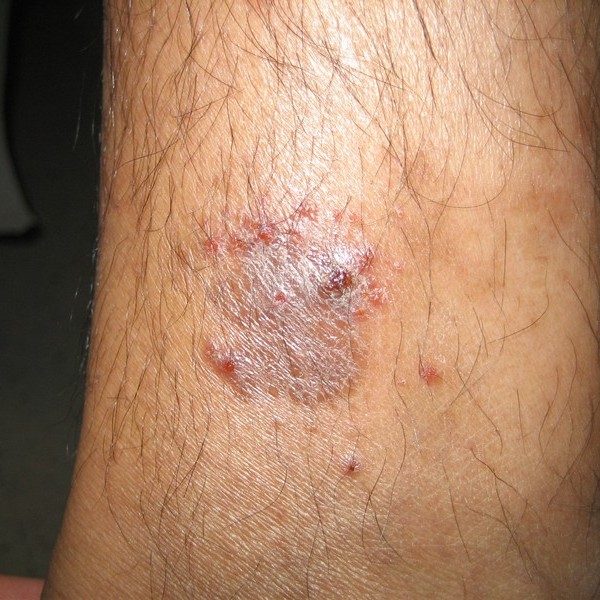
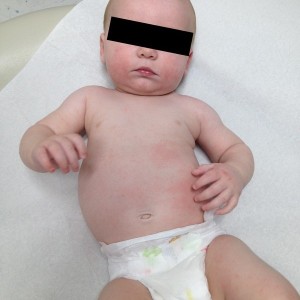
If you have itchy, red, bumpy, sometimes weepy and scaly skin that you just have to scratch along with seasonal allergies and/or problems with breathing, bronchitis, or asthma, or relatives with similar problems, you probably have eczema (atopic dermatitis). Rash of atopic dermatitis develops usually on scalp (babies), cheeks (babies), in front of the elbows, on wrists, hands, behind knees, around ankles and feet, or in more severe cases everywhere. Scratching can cause scarring and skin infections with yellowish crusting and weeping. But you should see your health care provider to confirm the diagnosis.
When should I see my health care provider for an eczema (atopic dermatitis)?
You should see your health care provider to have an initial exam, and to have the correct diagnosis. You should immediately report to your health care provider if you have any sudden worsening of your eczema, since it can be a sign of infection either bacterial or viral (herpes) that should be treated as soon as possible.
How will my health care provider know that I have an eczema?
There is no test that will tell you decisively that you have eczema; however, your health care provider can tell if you have an eczema examining your skin and by asking you questions. A skin biopsy is rarely necessary.
What is the treatment for eczema (atopic dermatitis)?
If you believe in the theory of problems with skin evaporating too much of water (see above), then wetting the skin with water followed with plain white petrolatum (brand name: Vaseline) and/or plain white petrolatum medicated with corticosteroids (medications that calm down the irritation and excessive immune reaction of the skin) should help with itching and eczema. Guess what- the above regimen does help, since wetting returns water back into the skin and plain white petrolatum or plain white petrolatum medicated with corticosteroids seal the water in the skin. This makes the skin softer, there is no dry scale to poke the skin, which in turn stops itching. Then scratching stops, and eczema stops getting worse. All of the above gives time for the skin to heal. This should be continued until eczema resolves, which happens in about half of children by the time they become adults (probably due to increased skin oil production during puberty which then seals the water in the skin). Also, try to avoid things that can make eczema worse, such as dry air, harsh soaps or any unnecessary cosmetic and hygienic preparations.
In addition to the above measures it is necessary to reduce microbes on the skin and fingernails that worsen eczema. For this we use diluted bleach baths (half a cup of regular bleach stirred into the half a bathtub of water), or CLn wash (shower gel with bleach: http://www.clnwash.com) 1-3 times weekly for 10-15 min to kill the microbes on the skin. Afterwards you should rinse your skin well and apply any prescribed ointment while your skin is still wet. This is necessary since various bacteria can worsen eczema and make it resistant to treatment. Sometimes antibiotic pills that you take by mouth are also necessary.
Moisturizing Ointments or Creams:
We only recommend plain white petrolatum (brand name: Vaseline), or for those who just do not like ointments – Vanicream. All should be used from tubes or pump dispensers and not form tubs or jars. Tubes are much more hygienic, since sticking fingers in the jar implants microbes into the ointment where they can flourish. In general we prefer ointments since they are much simpler compared to creams and usually do not have any preservatives, which sometimes can make your eczema worse.
Steroids:
Steroids are medications that calm down the irritation and excessive immune reaction of the skin. We usually prescribe generic ointments only (from weakest to strongest):
- Hydrocortisone 2.5% ointment (usually to the face, skin folds, genitalia),
- Desonide 0.05% ointment (usually to the face, skin folds, genitalia),
- Triamcinolone acetoinde 0.1% ointment (usually to the arms, legs, trunk with moderate severity),
- Betamethasone diproprionate 0.05% ointment (to the most severe and to the thickest areas),
- Clobetasol 0.05% ointment (to the most severe and to the thickest areas)
To scalp eczema we recommend fluocinolone 0.01% scalp solution for milder cases, and clobetasol 0.05% solution for the most severe cases.
If patient experiences side effects of steroid ointments (skin thinning, stretch marks), then we prescribe tacrolimus 0.03% or 0.1% ointment (brand name Protopic). However, this happens rarely in our practice.
When the eczema is widespread we recommend light therapy such as 10 minutes of natural sunlight daily to eczematous skin. If that is not possible, or without benefit, then we recommend narrow band ultraviolet B light (nbUVB) 3 times weekly (for this you have to come to a doctor’s office). When it is just not possible for patients to come three times weekly to doctor’s office, or when there is no such treatment option in the area, then we recommend visits to tanning salons with standing units, or we prescribe a personal home light box with help of two manufacturers of such nbUVB machines (Daavlin and National Biologics Corp.)
For severe cases we use triamcinolone acetoinde 0.1% ointment as body wet wraps for a week or two, which usually clears even the most severe eczemas. However, in the most severe and resistant cases we have to add immunosuppressive pills such as prednisone, azathioprine (brand name Imuran), methotrexate or mycofenolate mofetil (brand name CellCept).
If our patients have hard time sleeping from itching, then we add antihistamines such as hydroxyzine or doxepin pill.
Remember: the key is to keep the skin moist, or how health care providers like to say – well hydrated and moisturized!

What can I do to get rid of sores or abscesses that occur in armpit?
Dear Thulisule,
Having sores or abscesses in armpits is a serious problem for which you should see your physician as soon as possible.
You doctor may or may not do a swab for bacterial culture of sores/abscesses, may do incision and drainage,
and may prescribe you a course of antibiotics and/or diluted bleach baths.
All the best!
Dr. T
I was diagnosed of genital Herpes 6months ago and was in pain with the knowledge that there is no cure for the virus! there was a day I saw several post about a herbalist how he’s used natural herbal medicine to cure this particular virus, Immediately I contacted him on his website and he prepared and sent me the herbal medicine through DHL delivery and after 14days of usage, the Pain, and sores were gone i went to the hospital for test I’m the happiest woman on earth because I just tested negative to the virus! this testimony is real and thanks to Dr Ehiagwina you can also reach him on his Email: [email protected] or on whatsapp: +2348162084504.